Senior Reporter
Treating Sleep Apnea for Truck Drivers Remains a Thorny Issue
[Stay on top of transportation news: Get TTNews in your inbox.]
In the late 1990s, the safety team at Schneider began an experiment of sorts into the nettlesome problem of truck driver obstructive sleep apnea by first examining their drivers for such “comorbidity” conditions as heart disease, diabetes and gastrointestinal conditions.
At first, the company thought that perhaps such serious conditions were causing sleep apnea, recalls Tom DiSalvi, vice president of safety for the Green Bay, Wis.-based truckload, intermodal and logistics services provider.
“Then the recognition became, ‘No, it’s the sleep apnea that’s causing these medical conditions,’ ” DiSalvi said. “Because every time you stop breathing while you’re sleeping, it deprives your body of oxygen-rich blood, and that’s what causes these other medical issues.”
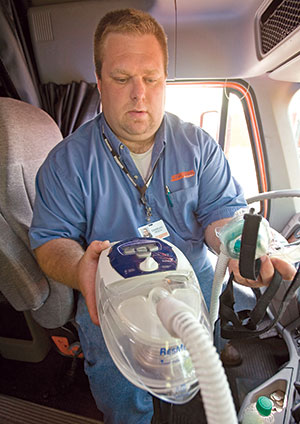
Drivers with sleep apnea can keep CPAP machines in their truck cabs to treat the condition. (Mike Roemer for Schneider National)
After several internal pilot projects, the company in 2006 began a first-of-its-kind sweeping program to identify those drivers at risk of apnea, sending them to clinics at locations nationwide for sleep studies and subsequent treatment — all at no cost to the drivers.
“In our minds, this was a win-win across the board,” DiSalvi said. “It was good for their long-term health, it was good for alertness and safety, and it was certainly the right thing to do.”
Over the years, the Schneider sleep apnea program, lauded in recent research studies as an effective way to identify and treat drivers with apnea and cut medical costs, has continued as a model method to address the potentially life-threatening and too often unrecognized and undiagnosed condition.
Researchers believe many truck drivers on U.S. highways have untreated sleep apnea, which remains a public safety danger and a serious driver health issue.
For years, diagnosing and treating sleep apnea has been a delicate and visceral dance among drivers, physicians, motor carriers and federal trucking regulators. Some drivers seemingly want to ignore the condition — or don’t know they have it — and physicians and trucking regulators have been in a tug of war over how it is diagnosed, treated and regulated, or not regulated. Most motor carriers seem to have been caught somewhere in the middle, not fighting regulation, but wanting the regulators to take into consideration the nature of their businesses.
According to the medical books, sleep apnea is a breathing-related sleep disorder that causes brief interruptions of breathing during sleep. These pauses in breathing can last at least 10 seconds or more and can occur up to 400 times a night, according to the Federal Motor Carrier Safety Administration. The result is not a restorative sleep.
It remains a major problem in the trucking industry because it can cause dangerous fatigue when drivers are behind the wheel. It also is a hot potato among some drivers due to the cost of sleep studies and complaints by others that some can’t tolerate the most effective treatment — using a continuous positive airway pressure machine, or CPAP.
The more common apnea risk factors identified by the medical review board include:
- Hypertension (treated or untreated)
- Type 2 diabetes (treated or untreated)
- A male neck size greater than 17 inches or female neck size greater than 15.5 inches
- A history of stroke, coronary artery disease or arrhythmias
- Loud snoring
- Hypothyroidism (underactive thyroid, untreated)
- Age 42 or older male or post-menopausal female
A problem with some CPAP machines hasn’t helped efforts to control the problem.
Last summer the U.S. Food and Drug Administration announced a voluntary recall by Philips Respironics Inc., a CPAP provider based in Murrysville, Pa., that has provided the machines used by up to an estimated 2 million drivers in the United States who were suddenly without their treatment. Since then, the company has been replacing the machines as fast as possible, but said in a recent statement all the replacements would not be completed until September. The masks were recalled due to a risk of exposure to harmful debris and chemicals, the company said.

CPAP equipment on display at an industry trade show. (John Sommers II for Transport Topics)
“When you look at the driving population now, the typical commercial motor vehicle driver is obese, over 40 and male, all risk factors for sleep apnea,” said Brian Morris, an M.D. who sits on FMCSA’s Medical Review Board.
Morris along with some other members of the agency’s medical review board have been loud voices in the fight to convince FMCSA to issue a formal rulemaking that would closely regulate and mandate medical examiners to follow strict protocols to screen drivers for apnea.
So far, that hasn’t happened.
“The last time we had a meeting [in September] the agency was going to refer to the work tweaked for the medical examiners handbook that we had done on sleep apnea, but making it clear that it wasn’t mandatory, that it was just a source of reference,” said Morris, corporate director of medical surveillance for Boston-based OccMed Consulting & Injury Care.
Should it be mandatory?
“Oh, yeah,” Morris said. “That’s what the board wanted way back when. It goes back so many years that I can’t even speculate how long ago it was — but at least five years ago or longer.”
Morris argues that not having tighter regulatory screening guidelines “pretty much leaves everything up to the certified medical examiner, which can be tough.”
“Some of the examiners have zero training in sleep apnea and essentially know nothing about it,” Morris added.
Years ago, it appeared that FMCSA was moving toward adopting regulatory mandates, issuing a proposed joint rule with the Federal Railroad Association in March 2016. Then in August 2017, the two agencies withdrew the rule, saying, “the current safety programs addressing fatigue risk management are the appropriate avenues to address OSA.”
“OSA remains an ongoing concern for the agencies and the motor carrier and railroad industries because it can cause unintended sleep episodes and resulting deficits in attention, concentration, situational awareness and memory, thus reducing the capacity to safely respond to hazards when performing safety-sensitive duties,” the agency said when it dumped the proposed rule.
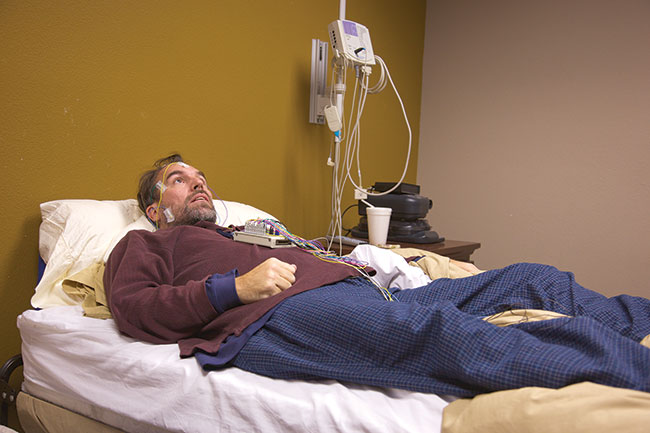
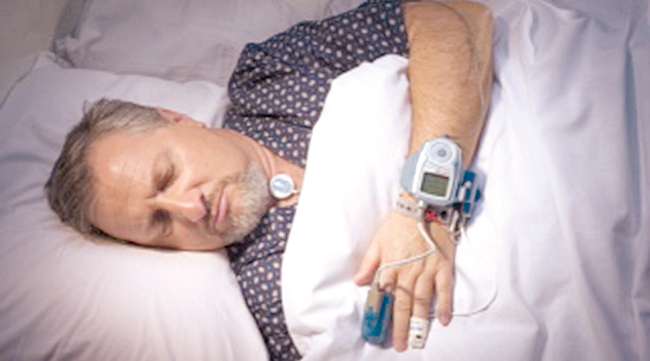
Sleep studies that measure pulse rate and sleep patterns can be used to diagnose sleep apnea. (pastorscott via Getty Images)
At that time, FMCSA reminded medical examiners that there are no rules or other regulatory guidance for screening, diagnosis and treatment of OSA in CMV drivers. “Medical certification determinations for such drivers are made by the examiners based on the examiner’s medical judgment rather than a federal regulation or requirement,” the agency said.
Since then, there have been no further attempts by FMCSA to take another shot at a rulemaking. The agency won’t really say why.
However, FMCSA said last summer that in lieu of a rulemaking, it is adding reference material in the medical examiner’s handbook that was provided by the medical review board to assist medical examiners with the screening process.
The handbook is being rewritten and was originally expected soon. However, in a statement to Transport Topics, FMCSA said it was still being revised and wouldn’t be made public until the end of 2022. When it is completed, it will be offered for public comment, the agency said.
FMCSA continues to say it does not have an estimate on the number of commercial vehicle drivers that may have sleep apnea.
“Previous research sponsored by the agency was inconclusive with regard to the number of drivers with moderate to severe OSA,” FMCSA said.
The agency declined to permit a reporter to discuss the issue with a subject-matter expert.

Learn about real-world adoption strategies for self-driving trucks with Robert Brown of Spartan Radar and Charlie Jatt of Waymo. Hear a snippet above, and get the full program by going to RoadSigns.TTNews.com.
“The current screening process has, at times, resulted in inconsistencies in the screening and diagnosis for obstructive sleep apnea as well as a lack of support for drivers needing treatment,” said Laura Spector, a safety policy specialist with American Trucking Associations.
“ATA supports the 2013 [congressional] bill that requires any action on obstructive sleep apnea screening to be done through a federal rulemaking process as compared to regulatory guidance,” Spector told TT. “If the agency moves forward with addressing OSA screening standards, the rulemaking process is necessary to ensure that the experience and insight of those in the industry can be incorporated into a new rule that makes sense for the industry while prioritizing safety.”
Schneider’s DiSalvi agrees. He said medical examiners are well trained, but thinks a regulation would help drive consistency.
“Because even with the training that the medical examiners receive, there’s still a degree of subjectivity,” DiSalvi said. “Whereas a regulation would be able to identify for the examiner if somebody has these health risk factors, then you send them to a sleep specialist. But I recognize that people are in different stages of support for this.”
A portion of the concern related to a more rigorous screening process comes from some independent owner-operators, who balk at the notion that they must spend their own money for a sleep study, which can cost thousands of dollars. They also fear they could lose their medical certifications or even be fired.
The answer to the sleep apnea problem is not as complicated as it might sound, said Mary Pat McKay, chief medical officer at the National Transportation Safety Board.
“We believe that all transportation operators, not just in highway, but also in other modes, should be screened and diagnosed and ensure that they have adequate treatment if they have sleep apnea,” McKay told TT. “It’s very simple. We know that sleep apnea increases crashes because of the fatigue associated with it.”
McKay added, “I know that truckers are worried that, ‘If I get diagnosed, I’ll be fired.’ No, that’s not true. The only time someone would be taken out of service for a diagnosis of sleep apnea is if they had a crash associated with fatigue. Fatigue associated with untreated sleep apnea increases crash risk.”
McKay said NTSB believes FMCSA should do a rulemaking for apnea.
“From a medical standpoint, this ain’t hard stuff,” she said. “This is straightforward. The treatment is non-invasive.”
Dan Horvath, vice president of safety policy for ATA, said unaddressed moderate to severe sleep apnea has the potential to be a safety concern for drivers and fleets.
However, Horvath added that because of the complexity of the issues involved, if FMCSA intends to address the potential dangers of sleep apnea through a rulemaking, it must balance the costs and benefits of a robust screening and treatment program.
At the same time, Horvath said when the agency establishes standards for certified medical examiners, it must also set “reasonable timelines for drivers between screening and diagnoses, provide flexibility with screening and treatment methods, and consider the diversity and complexities of motor carrier operations.”
Want more news? Listen to today's daily briefing above or go here for more info
In October the Commercial Vehicle Safety Alliance hired a sleep specialist, and in December announced it had agreed to take over as the home of the North American Fatigue Management Program, a comprehensive educational and training program aimed at preventing fatigue-related risks and crashes and cultivating a corporate safety culture that proactively works to eliminate driver fatigue.
Rodolfo Giacoman, the CVSA fatigue management program specialist, said carriers should do several things to get involved in the program, including establishing a sleep disorder screening and treatment program and fatigue risk management system to identify which of their drivers may be having drowsy driving incidents on the road.
Giacoman said a CVSA webinar is planned for May 4 to outline the fatigue program.
“We’re not taking a lead in the program,” said Collin Mooney, CVSA’s executive director. “We’re just managing the contract. The content still resides with the sleep experts.”

